Atrial fibrillation (AF) is a common arrhythmia affecting millions worldwide. It is characterized by an irregular heartbeat originating from the heart’s upper chambers (atria). AF can have significant health consequences, including an increased risk of stroke, heart failure, and mortality. Therefore, early diagnosis and appropriate management are essential. In this article, we will discuss the diagnosis of AF, including the clinical presentation, diagnostic tests, and management options.

Clinical Presentation:
AF can present with a range of symptoms, from mild to severe. The most common symptoms of AF include palpitations, shortness of breath, fatigue, dizziness, and chest discomfort. Some patients may not have symptoms and may only be diagnosed incidentally during a routine medical examination or an electrocardiogram (ECG).
AF can be classified into paroxysmal, persistent, or permanent based on the duration and pattern of episodes. Paroxysmal AF refers to episodes that terminate spontaneously within seven days. Persistent AF lasts longer than seven days and requires medical intervention to restore normal rhythm. Permanent AF is defined as continuous AF that is not amenable to rhythm control interventions.
Diagnostic Tests:
The diagnosis of AF is usually made based on clinical presentation and ECG findings. The ECG is the gold standard for diagnosing AF and can confirm the presence of an irregularly irregular rhythm with absent P waves. The ECG can also identify the type of AF (paroxysmal, persistent, or permanent) and any underlying structural heart disease. Below is a representative ECG strip that shows an irregular rhythm that is consistent with atrial fibrillation.

In some cases, additional tests may be necessary to evaluate the underlying cause of AF and to assess the risk of thromboembolism. These tests may include:
Echocardiography: This is an ultrasound test that provides detailed images of the heart’s structure and function. Echocardiography can identify any underlying structural heart disease, such as valvular heart disease, left ventricular hypertrophy, or atrial enlargement, which can increase the risk of AF. In particular, rheumatic heart disease precipitates AF, especially in women. Rheumatic heart disease often affects third-world countries, caused by strep infection of the pharynx that leads to degenerative causes of the mitral valve. Furthermore, AF can also cause congestive heart failure; therefore, an echocardiogram can help screen patients at risk for sudden cardiac death.
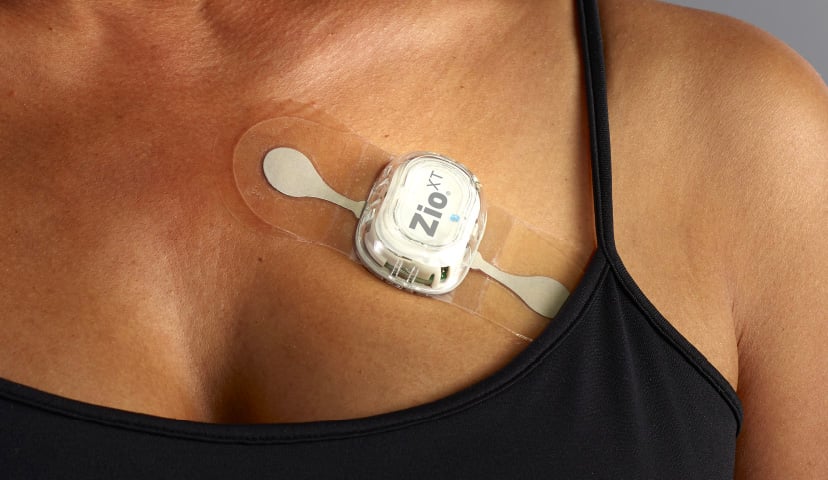
Holter Monitor: This portable ECG device records the heart’s rhythm for 24 to 48 hours. It can be useful in diagnosing paroxysmal AF and assessing the frequency and duration of episodes. The above picture is a Ziopatch device that can record up to 1-2 weeks of cardiac rhythms to help detect any signs of AF/ aflutter/ AVNRT/ and others. It is also a patient trigger system that allows you to notify the clinician when you are experiencing symptoms.

Event Recorder: This is a device that is similar to a Holter monitor but can be worn for a more extended period (up to 2 years) to capture intermittent symptoms of AF. It is invasive, and it requires a clinician who knows how to insert this device into the anterior portion of the chest. It will remain in your body for up to several years, and it helps to capture symptoms that are irregular.
Blood Tests: These tests can assess the patient’s overall health and identify any underlying medical conditions, such as thyroid dysfunction or electrolyte abnormalities, that can contribute to the development of AF. The most common cause of AF is, by far, obstructive sleep apnea and chronic hypertension. However, sometimes blood tests can be overlooked, and patients should have a complete set of blood work during the evaluation for AF.
By employing the above testing strategies, the providers can help risk stratify your health and treat you according to the cause of your AF. It also can help providers decide which medication will work best for you, as personalized medicine is the most effective way to treat AF in this era. In the next article, we will be talking about the common management plans for atrial fibrillation as well as preventive care and risk factors.
Please note that the above information is for medical education purposes only; if you have an emergency, please contact your physician or visit the nearby emergency department for help.
For my list of self-improvement items, check out the books that I recommend,
Rich Dad, Poor Dad: https://amzn.to/39d33lT
The 7 Habits of Highly Effective People: https://amzn.to/3M7JM3K
The Emporer of All Maladies: https://amzn.to/39Gj2ca
Gifted hands:https://amzn.to/38kp1mL
The Power of Habits: https://amzn.to/3MpwHmk
Cook County ICU Interesting Cases: https://amzn.to/3lgzpPp
For USMLE step exam prep books, I recommend:
First Aid Step 1: https://amzn.to/3lyKxXR
First Aid Step 2 CK: https://amzn.to/3G9eYNM
Master the Board Step 3: https://amzn.to/3ly5uCiA
Share this:
- Share on X (Opens in new window) X
- Share on Facebook (Opens in new window) Facebook
- Print (Opens in new window) Print
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Reddit (Opens in new window) Reddit
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on Telegram (Opens in new window) Telegram
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email